The word “condyloma” comes from the Greek word meaning “knob.”
Any knob-like or warty growth on the genitals is known as a condyloma. Venereal warts caused by human papilloma virus are known as “condyloma accuminata”. The skin lesions caused by Molitor hominus are known as “condyloma subcutaneum” (molluscum contagiosum). The skin lesions associated with secondary syphilis are called “condyloma lata.”
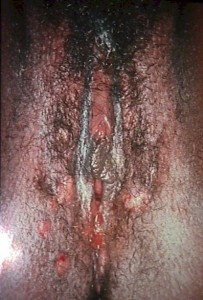
They have in common with veneral warts the fact that they are both raised lesions on the vulva (or penis), but there ends the similarity.
- condyloma accuminata are cauliflower-like, while condyloma lata are smooth.
- condyloma accuminata are dry, while condyloma lata are moist.
- condyloma accuminata are bulky while, condyloma lata are flat.
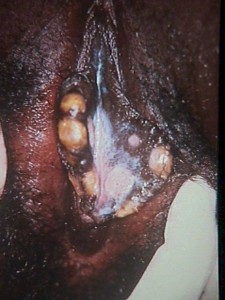
Examination of surface scrapings of condyloma lata lesions under darkfield microscopy will show the typical spirochetes. Serologic test for syphilis (VDRL, RPR) will be positive.
Primary and Secondary Syphilis*
Treatment
Parenteral penicillin G has been used effectively to achieve clinical resolution (i.e., the healing of lesions and prevention of sexual transmission) and to prevent late sequelae. However, no comparative trials have been conducted to guide the selection of an optimal penicillin regimen. Substantially fewer data are available for nonpenicillin regimens.
Recommended Regimen for Adults
Benzathine penicillin G 2.4 million units IM in a single dose
*Recommendations for treating syphilis in persons with HIV infection and pregnant women are discussed elsewhere in this report (see Syphilis among Persons with HIV infection and Syphilis During Pregnancy).
Available data demonstrate that use of additional doses of benzathine penicillin G, amoxicillin, or other antibiotics do not enhance efficacy when used to treat primary and secondary syphilis, regardless of HIV status.
Recommended Regimen for Infants and Children
Benzathine penicillin G 50,000 units/kg IM, up to the adult dose of 2.4 million units in a single dose
Infants and children aged >1 month who receive a diagnosis of syphilis should have birth and maternal medical records reviewed to assess whether they have congenital or acquired syphilis (see Congenital Syphilis). Infants and children aged ≥1 month with primary and secondary syphilis should be managed by a pediatric infectious-disease specialist and evaluated for sexual abuse (e.g., through consultation with child-protection services) (see Sexual Assault or Abuse of Children).
Other Management Considerations
All persons who have primary and secondary syphilis should be tested for HIV infection. In geographic areas in which the prevalence of HIV is high, persons who have primary or secondary syphilis should be retested for acute HIV in 3 months if the first HIV test result was negative.
Persons who have syphilis and symptoms or signs suggesting neurologic disease (e.g., cranial nerve dysfunction, meningitis, stroke, and hearing loss) or ophthalmic disease (e.g., uveitis, iritis, neuroretinitis, and optic neuritis) should have an evaluation that includes CSF analysis, ocular slit-lamp ophthalmologic examination, and otologic examination. Treatment should be guided by the results of this evaluation.
Invasion of CSF by T. pallidum accompanied by CSF laboratory abnormalities is common among adults who have primary or secondary syphilis. In the absence of clinical neurologic findings, no evidence supports variation from the recommended treatment regimen for primary and secondary syphilis. Symptomatic neurosyphilis develops in only a limited number of persons after treatment with the penicillin regimens recommended for primary and secondary syphilis. Therefore, unless clinical signs or symptoms of neurologic or ophthalmic involvement are present, routine CSF analysis is not recommended for persons who have primary or secondary syphilis.
Follow-Up
Clinical and serologic evaluation should be performed at 6 and 12 months after treatment; more frequent evaluation might be prudent if follow-up is uncertain or if repeat infection is a concern. Serologic response (i.e., titer) should be compared with the titer at the time of treatment. However, assessing serologic response to treatment can be difficult, and definitive criteria for cure or failure have not been well established. In addition, nontreponemal test titers might decline more slowly for persons previously treated for syphilis .
Persons who have signs or symptoms that persist or recur and those with at least a fourfold increase in nontreponemal test titer persisting for >2 weeks likely experienced treatment failure or were re-infected. These persons should be retreated and reevaluated for HIV infection. Because treatment failure usually cannot be reliably distinguished from reinfection with T. pallidum, a CSF analysis also should be performed; treatment should be guided by CSF findings.
Failure of nontreponemal test titers to decline fourfold within 6–12 months after therapy for primary or secondary syphilis might be indicative of treatment failure. However, clinical trial data have demonstrated that 15%–20% of persons with primary and secondary syphilis treated with the recommended therapy will not achieve the fourfold decline in nontreponemal titer used to define response at 1 year after treatment. Serologic response to treatment appears to be associated with several factors, including the person’s stage of syphilis (earlier stages are more likely to decline fourfold and become negative) and initial nontreponemal antibody titers (lower titers are less likely to decline fourfold than higher titers) (409). Optimal management of persons who have less than a fourfold decline in titers after treatment of syphilis is unclear. At a minimum, these persons should receive additional clinical and serologic follow-up and be evaluated for HIV infection. If additional follow-up cannot be ensured, retreatment is recommended. Because treatment failure might be the result of unrecognized CNS infection, CSF examination can be considered in such situations.
For retreatment, weekly injections of benzathine penicillin G 2.4 million units IM for 3 weeks is recommended, unless CSF examination indicates that neurosyphilis is present (see Neurosyphilis). Serologic titers might not decline despite a negative CSF examination and a repeated course of therapy. In these circumstances, although the need for additional therapy or repeated CSF examinations is unclear, it is not generally recommended.
Penicillin Allergy
Data to support use of alternatives to penicillin in the treatment of primary and secondary syphilis are limited. However, several therapies might be effective in nonpregnant, penicillin-allergic persons who have primary or secondary syphilis. Regimens of doxycycline 100 mg orally twice daily for 14 days and tetracycline (500 mg four times daily for 14 days) have been used for many years. Compliance is likely to be better with doxycycline than tetracycline, because tetracycline can cause gastrointestinal side effects and requires more frequent dosing.
Although limited clinical studies, along with biologic and pharmacologic evidence, suggest that ceftriaxone (1–2 g daily either IM or IV for 10–14 days) is effective for treating primary and secondary syphilis, the optimal dose and duration of ceftriaxone therapy have not been defined.
Azithromycin as a single 2-g oral dose has been effective for treating primary and secondary syphilis in some populations. However, T. pallidum chromosomal mutations associated with azithromycin and other macrolide resistance and treatment failures have been documented in multiple geographical areas in the United States. Accordingly, azithromycin should not be used as first-line treatment for syphilis and should be used with caution only when treatment with penicillin or doxycycline is not feasible. Azithromycin should not be used in MSM, persons with HIV, or pregnant women. Careful clinical and serologic follow-up of persons receiving any alternative therapies is essential.
Persons with a penicillin allergy whose compliance with therapy or follow-up cannot be ensured should be desensitized and treated with benzathine penicillin. Skin testing for penicillin allergy might be useful in some circumstances in which the reagents and expertise are available to perform the test adequately (see Management of Persons Who Have a History of Penicillin Allergy).
Pregnancy
Pregnant women with primary or secondary syphilis who are allergic to penicillin should be desensitized and treated with penicillin. For more information, see Management of Persons Who Have a History of Penicillin Allergy and Syphilis During Pregnancy.
Special Considerations
Pregnancy
Parenteral penicillin G is the only therapy with documented efficacy for syphilis during pregnancy. Pregnant women with syphilis in any stage who report penicillin allergy should be desensitized and treated with penicillin (see Management of Persons Who Have a History of Penicillin Allergy).
Jarisch-Herxheimer Reaction
The Jarisch-Herxheimer reaction is an acute febrile reaction frequently accompanied by headache, myalgia, fever, and other symptoms that can occur within the first 24 hours after the initiation of any therapy for syphilis. Patients should be informed about this possible adverse reaction and how to manage it if it occurs. The Jarisch-Herxheimer reaction occurs most frequently among persons who have early syphilis, presumably because bacterial burdens are higher during these stages. Antipyretics can be used to manage symptoms, but they have not been proven to prevent this reaction. The Jarisch-Herxheimer reaction might induce early labor or cause fetal distress in pregnant women, but this should not prevent or delay therapy (see Syphilis During Pregnancy).
Management of Sex Partners
Sexual transmission of T. pallidum is thought to occur only when mucocutaneous syphilitic lesions are present. Such manifestations are uncommon after the first year of infection. Persons exposed sexually to a person who has primary, secondary, or early latent syphilis should be evaluated clinically and serologically and treated according to the following recommendations:
- Persons who have had sexual contact with a person who receives a diagnosis of primary, secondary, or early latent syphilis within 90 days preceding the diagnosis should be treated presumptively for early syphilis, even if serologic test results are negative.
- Persons who have had sexual contact with a person who receives a diagnosis of primary, secondary, or early latent syphilis >90 days before the diagnosis should be treated presumptively for early syphilis if serologic test results are not immediately available and the opportunity for follow-up is uncertain. If serologic tests are negative, no treatment is needed. If serologic tests are positive, treatment should be based on clinical and serologic evaluation and stage of syphilis.
- In some areas or populations with high rates of syphilis, health departments recommend notification and presumptive treatment of sex partners of persons with late latent syphilis who have high nontreponemal serologic test titers (i.e., >1:32), because high titers might be indicative of early syphilis. These partners should be managed as if the index case had early syphilis.
- Long-term sex partners of persons who have late latent syphilis should be evaluated clinically and serologically for syphilis and treated on the basis of the evaluation’s findings.
- The following sex partners of persons with syphilis are considered at risk for infection and should be confidentially notified of the exposure and need for evaluation: partners who have had sexual contact within 1) 3 months plus the duration of symptoms for persons who receive a diagnosis of primary syphilis, 2) 6 months plus duration of symptoms for those with secondary syphilis, and 3) 1 year for persons with early latent syphilis.
*CDC 2015 STD Treatment Guidelines
