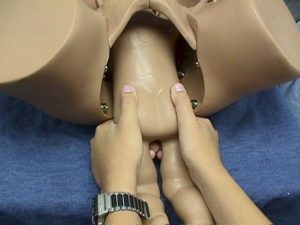
The simplest breech delivery is called a spontaneous breech.
The mother pushes the baby out with the normal bearing down efforts and the baby is simply supported until it is completely free of the birth canal. These babies pretty much deliver themselves.
This works best with smaller babies, mothers who have delivered in the past, and frank breech presentation.
Assisted Breech Delivery
If the breech baby gets stuck half-way out, or if there is a need to speed the delivery, an “assisted breech” delivery may be necessary. For this type of delivery, it is very helpful to have:
- At least one qualified assistant,
- An anesthetist or anesthesiologist in the event general anesthesia is needed, and
- Someone skilled in neonatal resuscitation other than yourself.
The wisest of obstetricians has these individuals present for all breech deliveries.
Make sure you have a generous episiotomy. This will give you more room to work, but may be unnecessary if the vulva is very stretchy and compliant. Otherwise, you can make an episiotomy, enlarge a pre-existing episiotomy, surgically (with scissors) extend a pre-existing perineal laceration, or make a second episiotomy. Some physicians will intentionally extend an episiotomy into the rectum (“proctoepisiorrhaphy”) because it gives them lots of room, is relatively easy to repair after the delivery, and rarely leads to any long-term problems for the mother.
Grasp the baby so that your thumbs are over the baby’s hips. If you grasp the baby any higher than that, there is some risk of injury to the fetal kidneys and abdominal organs.
If the baby is not facing “face down,” gently rotate the torso so the baby is face down in the birth canal (facing toward the maternal rectum).
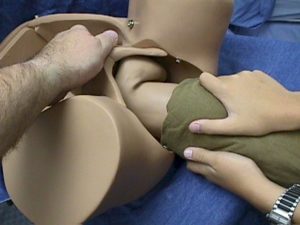
Wrap a towel around the hips and legs. It will provide a more secure grip and will keep the legs secure and out of the way.
Have your assistant apply suprapubic pressure to keep the fetal head flexed.
Exert gentle outward traction on the baby while rotating the baby first clockwise and then counterclockwise a few degrees to free up the arms.
If the arms are trapped in the birth canal, you may need to reach up along the side of the baby and sweep them, one at a time, across the chest and out of the vagina. (More on this later.)
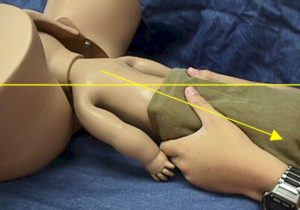
Keep the baby’s body at or below the horizontal plane or axis of the birth canal.
If you bring the baby’s body above the horizontal axis, you risk injuring the baby’s spine through hyperextension.
Only when the baby’s nose and mouth are visible at the introitus is it wise to bring the body up. At this point, you can visually see the attitude of the fetal head and avoid hyperextension.
The application of suprapubic pressure by the assistant is important for keeping the head flexed against the chest, expediting delivery, and reducing the risk spinal injury.
At this stage, the baby is still unable to breath and the umbilical cord is likely occluded.
Without rushing, move steadily toward a prompt delivery.
Placing your finger in the baby’s mouth may help you control the delivery of the head.
Try not to let the head “pop” out of the birth canal. A slower, controlled delivery is less traumatic.
Entrapped Head
Sometimes, after delivery of the fetal torso and arms, the head remains trapped, unable to pass through the cervix. This is a problem that must be promptly resolved.
- If the cervix is stretchy enough, increased pushing efforts by the mother and suprapubic pressure by an assistant can overcome mild head entrapment and lead to prompt delivery.
- If the cervix is not stretchy enough, or there is more than mild degrees of head entrapment, it will be necessary to cut the cervix longitudinally (Dührson’s Incisions) to quickly enlarge the cervical opening before the fetus is compromised. After delivery, you can repair the cervix. The traditional recommendation for these incisions is at about 10 o’clock and 2 o’clock, but anywhere you can get enough exposure will likely work.
Nuchal Arms
Normally during a breech delivery, the fetal arms remain flexed across the chest and deliver with the fetal torso. Arm entrapment (nuchal arms) occurs when the arms become raised up over the fetal head. Not only must the head pass through the cervix, but the added bulk of one or two arms must come with it. If the cervix is stretchy enough, normal delivery may still occur spontaneously.
In other cases, you must:
- Reach up,
- Identify the shoulder blade
- Follow the humerus as far up to the elbow as you flex the arm, sweeping the extended arm down, across the chest and out of the vagina.
If both arms are trapped, then you must perform this maneuver twice, once for each arm. There are dangers in performing this maneuver, of course. You may dislocate the fetal shoulder, or fracture the shoulder, collarbone, or humerus. Try to be gentle in performing this maneuver to avoid injury to the fetus. Remember, though, that failure to resolve this problem will result in fetal death, so it is important to use that degree of force necessary to deliver the fetus.