|
|
Lesson 3: Catheterization of the Male and Female Patient
Catheterization of the urinary bladder is the insertion of a hollow tube through the urethra into the bladder for removing urine. It is an aseptic procedure for which sterile equipment is required.
3-2. PURPOSES OF URINARY CATHETERIZATION
Purposes for urinary catheterization include the following.
a. Relieve Urinary Retention. Urine retained in the bladder for any reason causes the patient discomfort and increases the likelihood of infection. A catheter may be inserted to relieve urinary retention when a patient is temporarily unable to void or has difficulty releasing urine from the bladder due to an obstruction of the urethra or at the meatus.
b. Obtain a Sterile Urine Specimen from a Female Patient. At one time, this was considered necessary to obtain a urine specimen entirely free of contamination. Most physicians now order a collection of a voided, midstream clean-catch specimen.
c. Measure Residual Urine. Catheterization can be done to measure the amount of residual urine in the bladder when voiding only partly empties it.
d. Empty the Bladder Before, During, or After Surgery. A catheter may be inserted before or following abdominal surgery, especially if the patient cannot be up and about. Catheterization to keep the bladder empty of urine during a surgical procedure permits the surgeon a better view and palpation of internal tissue, and prevents accidental injury to the bladder. Catheterization may also be used to prevent urine from touching sutures in the perineum.
The French scale (Fr.) is used to denote the size of catheters. Each unit is roughly equivalent to 0.33 mm in diameter (that is, 18 Fr. indicates a diameter of 6 mm). The smaller the number, the smaller the catheter. A larger sized catheter is used for a male because it is stiffer, thus easier to push the distance of the male urethra. Catheters come in several sizes:
a. Number 8 Fr. and 10 Fr. are used for children.
b. Number 14 Fr. and 16 Fr. are used for female adults.
c. Number 20 Fr. and 22 Fr. are usually used for male adults.
3-4. TYPES OF URINARY CATHETERS
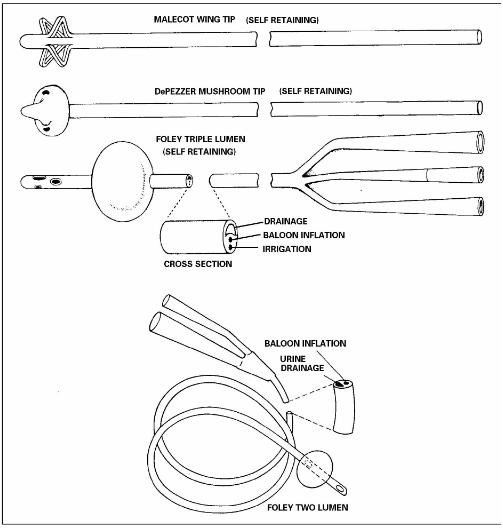
The catheters most commonly used are made of plastic. Each type of catheter (figure 3-1) has a rounded tip to prevent injury to the meatus or the urethra. The Foley catheter is frequently used. It is usually inserted by the nurse. The Malecot four-wing catheter and the dePezzer mushroom catheter are inserted by the urologist using a stylet. The stylet is removed after the catheter has been inserted. Because they are very difficult to sterilize, catheters should be considered disposable and discarded after they have been removed.
Figure 3-1. Urinary catheters.
a. Intermittent Catheter. An intermittent catheter is used to drain the bladder for short periods (5-10 minutes). It may be inserted by the patient.
b. Retention/Indwelling Catheter. This type of catheter is placed into the bladder and secured there for a period of time. It is used following surgery, bladder injury, or in bladder infections. It may also be used for an incontinent or nonresponsive patient.
(1) It provides continuous temporary or permanent drainage of urine.
(2) It is used for gradual decompression of an over distended bladder.
(3) It is used for intermittent drainage and irrigation.
(4) The most commonly used indwelling catheter is the Foley catheter. A drainage tube and collection device are connected to the catheter. It has a balloon at the distal end, which is inflated with sterile water or saline to prevent the catheter from slipping out of the bladder. It is multi-lumened (having several passages within the catheter). One lumen provides a passage for fluid to inflate the balloon. This passage may be self-sealing or may require a clamp. The second lumen is the passage through which the urine drains. Some indwelling catheters have a third lumen for instilling irrigation fluid.
c. Supra Pubic Catheter. This type of catheter is inserted into the bladder through a small incision above the pubic area. It is used for continuous drainage.
3-5. PREPARING FOR CATHETERIZATION
A catheter should be used only when absolutely necessary and the catheterization procedure itself should be done only by trained personnel under sterile conditions. Infection is a major risk of urinary catheterization.
a. Gather All Equipment.
(1) Disposable indwelling catheter kit. The kit contains the required equipment needed for catheterization and is packaged to ensure that the equipment is sterile. The kit includes the catheter, a drape, a receptacle to receive urine, materials to clean the area of insertion, a lubricant, a specimen container, and sterile gloves.
(2) Flashlight or lamp.
(3) Urine collection bag.
(4) Velcro leg strap or anchoring tape.
(5) Disposal bag.
(6) Waterproof pad or Chux®.
b. Explain the Procedure to the Patient. Advise the patient that he may feel a burning sensation and pressure as the catheter is inserted, and that he will feel that he needs to void after the catheter is in place. Do not suggest to the patient that he may feel pain; however, introducing a catheter in swollen or injured tissue may cause discomfort.
c. Provide for Privacy and Adequate Lighting.
(1) Close the door or pull the curtain surrounding the patient's bed and position the flashlight or lamp at the end of the bed.
(2) Position the female patient in a dorsal recumbent position with the knees flexed and the feet about two feet apart. Place Chux® under the patient's buttocks. Cover the upper body and each leg. Place the catheter set between the female patient's legs.
(3) Position a male patient in a supine position. Place Chux® under the patient's buttocks. Drape the patient so that only the area around the penis is exposed. Place the catheter set next to the legs of the male patient.
3-6. INSERTING THE FOLEY CATHETER IN A MALE PATIENT
The following procedures are used to insert the Foley catheter in a male patient.
a. Cleanse the genital and perineal areas with warm soap and water. Rinse and dry.
b. Wash your hands carefully.
c. Open the sterile catheterization kit, using sterile technique.
d. Put on the sterile gloves.
e. Open the sterile drape and place on the patient's thighs. Place fenestrated drape with opening on the penis.
f. Apply sterile lubricant liberally to the catheter tip. Lubricate at least six inches of the catheter. Leave the lubricated catheter on the sterile field.
g. Pour the antiseptic solution over the cotton balls.
h. Place the urine specimen collection container within easy reach.
i. Grasp the patient's penis between your thumb and forefinger of your nondominant hand. Retract the foreskin of an uncircumcised male. The gloved hand that has touched the patient is now contaminated.
|
|
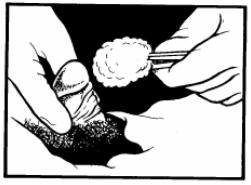
j. Use the forceps to hold the cotton balls (figure 3-2). This will maintain the sterility of one hand. Using the forceps, pick up one cotton ball and swab the center of the meatus outward in a circular manner.
k. Continue outward, using a new cotton ball for each progressively larger circle. Clean the entire glands. Deposit each cotton ball in the disposal bag. After the last cotton ball is used, drop the forceps into the disposal bag as well.
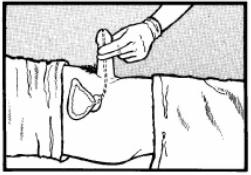
l. Hold the penis at a 90-degree angle (figure 3-3). Advance the catheter into the patient's urinary meatus. You may encounter resistance at the prostatic sphincter.
(1) Pause and allow the sphincter to relax.
(2) Lower the penis and continue to advance the catheter.
NOTE: Never force the catheter to advance. Discontinue the procedure if the catheter will not advance or the patient has unusual discomfort. Get assistance from the charge nurse or physician.
m. When the catheter has passed through the prostatic sphincter into the bladder, urine will start to flow into the collection bag if it is preconnected. If it is not preconnected, collect a specimen if required, then place the end of the catheter into the tubing of the sterile receptacle.
n. Attach the syringe to the balloon port and inject the water slowly to inflate the balloon. Connect the urine collection bag if it is not preconnected.
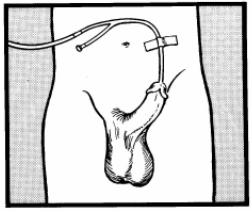
o. Anchor the catheter tubing to the lateral abdomen with tape (figure 3-4).
p. Secure the urinary collection bag below the level of the bladder and off the floor. Coil any extra tubing on the bed.
q. Remove your gloves, the drapes and protectors from around the patient, and any lubricant or antiseptic on the patient's skin.
r. Discard disposable equipment and return reusable equipment to the appropriate area.
s. Record the time that the procedure was done and by whom, the patient's reaction to the procedure, all patient teaching done and the patient's level of understanding. Report any significant observations to the charge nurse to include:
(1) The amount, color, and clarity of the urine.
(2) Any difficulties with the procedure.
(3) The presence of blood in the urine.